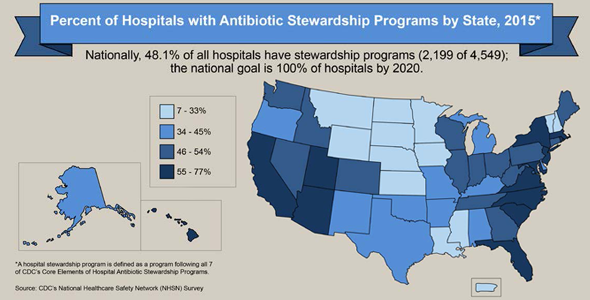
According to the CDC’s report, Antibiotic Use in the United States: Progress and Opportunities, released earlier this year, progress is mixed toward the CDC’s goal of one hundred percent adoption of antibiotic stewardship programs in hospitals (ASPs) by 2020. Some states have made more progress than others, with adoption rates ranging between 7% and 77%.
Implementing an effective ASP, which is a key component for improving prescribing practices and fighting antibiotic resistance, comes with a variety of challenges for any hospital. However, the CDC found that large hospitals implemented all seven of its Core Elements at a much higher rate than small hospitals—66% of hospitals with more than two hundred beds, and 31% of hospitals with fewer than fifty beds. Therefore, states with more small, rural hospitals may face additional challenges when it comes to meeting ASP implementation goals, often due to limited resources.
The good news is that there are a variety of tools available to help meet small hospitals’ unique challenges. To support ASP implementation at small hospitals, the CDC partnered with The Pew Charitable Trusts, the American Hospital Association, and the Federal Office or Rural Health Policy to develop Implementation of Antimicrobial Stewardship Core Elements at Small and Critical Access Hospitals.
Further, there are also online courses available from both the CDC and the WHO, along with CIDRAP’s webinars, podcasts, news, and commentary. For those requiring a printed resource or who may be participating in an ESCMID study group on antibiotic policies (ESGAP), Antimicrobial Stewardship (AMS), Volume Two focuses on the most recent antimicrobial stewardship strategies that synthesize basic and clinical sciences.
Effective ASP adoption is never easy, but hospitals are continuing to make progress, with the CDC reporting a national increase in hospitals implementing all seven Core Elements.
Click Here for Additional Resources on Antimicrobial Stewardship
Opinions expressed in this article are not necessarily those of bioMérieux, Inc.