Sepsis is the body’s life-threatening, imbalanced response to a severe infection. The condition affects 1.7 million people and takes 270,000 lives in the U.S. every year. This year, we face additional risks because of the threat of COVID-19.
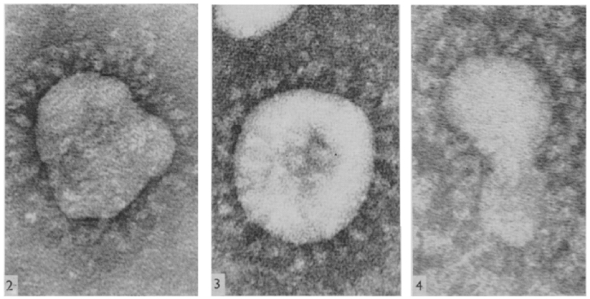
June Almeida & The Discovery of the First Human Coronavirus
Almeida’s contributions to the field of virology are immeasurable. Besides her discovery of the coronavirus family, she pioneered and perfected multiple techniques that have resulted in huge strides in viral imaging and diagnosis.
Decades of Progress Against the World’s Deadliest Diseases Could be Lost to the COVID-19 Pandemic
Three well-established infectious diseases—Tuberculosis, malaria, and HIV—are poised to kill millions worldwide, with decades of healthcare progress that could be lost due to disruptions caused by COVID-19. Even under normal circumstances, the toll these three diseases exact worldwide is staggering.
“On the Frontlines” Webinar Series, September 10—The Convergence of Microbiology and Pharmacy to Enhance Antibiotic Stewardship with Bloodstream Infections: The Need for Speed
A study published in June 2019 found that combining rapid blood culture identification (BCID) testing with antimicrobial stewardship initiatives yielded a decrease in broad spectrum antibiotic use.
The Value of Diagnostics in Combatting Antimicrobial Resistance – A Public Health Problem
At this year’s World Anti-Microbial Resistance Congress, Dr. Tristan Timbrook delivered a...
Lindsay Denny Discusses the Critical Role of WASH in Preventing Infectious Diseases and Fighting Antimicrobial Resistance
WASH, which stands for water, sanitation, and hygiene, are basic...