Updated September 2020.
By John Hurst, PharmD, BCPS-AQ ID, Senior Director, Antimicrobial Stewardship at bioMérieux and Mauricio Berdugo, MD, MPH, Director, Global Scientific & Medical Affairs at bioMérieux
Download the Cost of Sepsis Infographic
Sepsis, a potentially life-threatening condition caused by the body’s response to an infection, affects more than 1.7 million adults in the US a year. Sepsis can happen to anyone who has an infection, but it is most common in older adults, pregnant women, children younger than one, and those with chronic conditions or weakened immune systems.
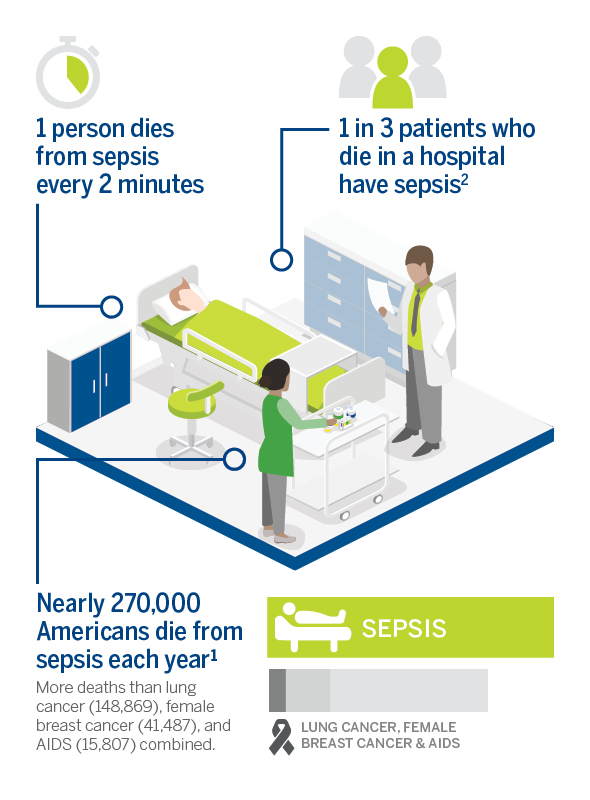
Over 270,000 lives are lost to sepsis each year in the United States. Prevention and early recognition of sepsis are of paramount importance in improving mortality rates.
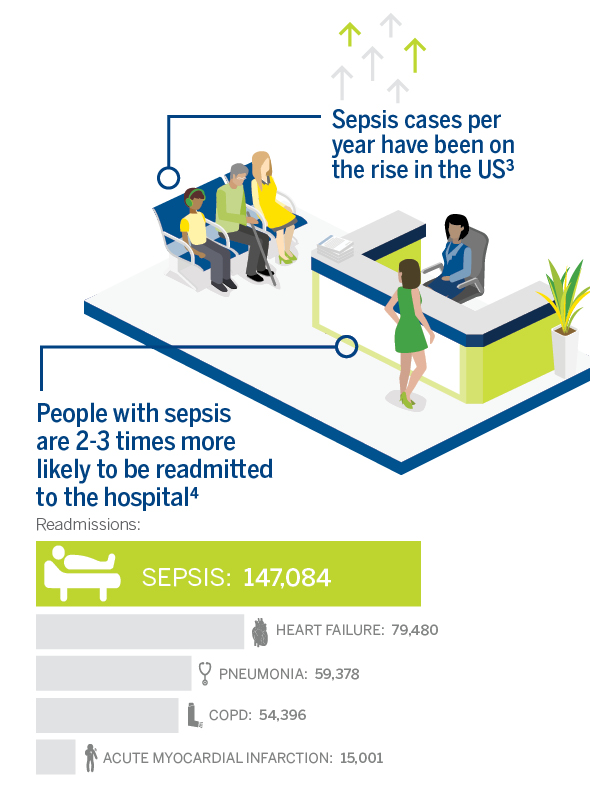
In addition to the toll sepsis takes on people’s lives, sepsis presents a major financial burden to US healthcare systems. According to a recent report published by Premier, from 2015 to 2018, the cost of treating patients who develop sepsis in the hospital rose by 20%, with hospitals spending $70,000 per case in 2018.
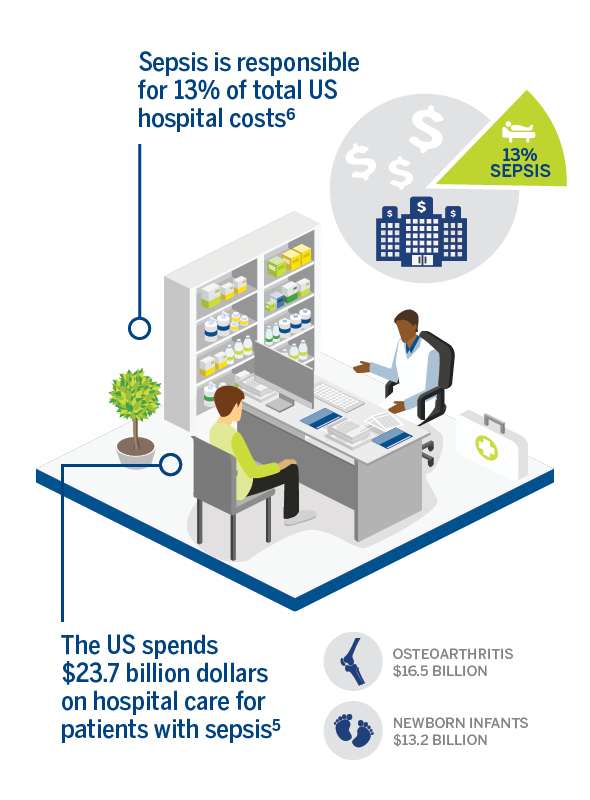
Dr. Madeleine Biondolillo, Vice President of Quality Innovation at Premier, said that septic shock is probably more common among patients already in the hospital because they often have weakened immune systems. Septic shock is the most serious complication of sepsis and is associated with high mortality rates.

The Centers for Medicare and Medicaid Services (CMS) require hospitals to comply with a sepsis bundle and initiate treatment within three- and six-hour time frames. However, the national average compliance rate is only 51%.
To alleviate the burden of sepsis on patients, families, and the healthcare system, everyone must take or continue to take impactful actions according to their roles, raising awareness, fighting infectious diseases, and improving patient outcomes.
References:
- Rhee C, Dantes R, Epstein L, et al. Incidence and Trends of Sepsis in US Hospitals Using Clinical vs Claims Data, 2009-2014. JAMA. 2017;318(13):1241. doi:10.1001/jama.2017.13836.
- Data & Reports | Sepsis | CDC. Centers for Disease Control and Prevention. https://www.cdc.gov/sepsis/datareports/index.html. Published August 23, 2016. Accessed August 14, 2019.
- Gaieski DF, Edwards JM, Kallan MJ, Carr BG. Benchmarking the Incidence and Mortality of Severe Sepsis in the United States. Critical Care Medicine. 2013;41(5):1167-1174.
- Mary FB, Talisa VB, Balakumar V, Chang CH, Fine M, Yende S. Proportion and Cost of Unplanned 30-Day Readmissions After Sepsis Compared With Other Medical Conditions. JAMA. 2017;317(5):530-531. doi:10.1001/jama.2016.20468
- Torio C, Moore B. National Inpatient Hospital Costs: The Most Expensive Conditions by Payer, 2013. HCUP Statistical Brief 204. May 2016. Agency for the Healthcare Research and Quality, Rockville, MD. http://www.hcup-us.ahrq.go/reports/statbriefs/sb204-Most-Expensive-Hospital-Conditions.pdf.
- Paoli CJ, Reynolds MA, Sinha M, Gitlin M, Crouser E. Epidemiology and Costs of Sepsis in the United States – An Analysis Based on Timing of Diagnostics and Severity Level. Critical Care Medicine. 2018;46(12):1889-1897. doi:10.1097/cm.0000000000003342
- Castellucci M. Sepsis costs Medicare $6 billion in 2015, more than any other discharge. Modern Healthcare. https://www.modernhaelthcare.com/article/20170901/NEWS/170909982/sepsis-costs-medicare-6-billion-in-2015-more-than-any-otherdischarge. Published September 1, 2017. Accessed August 14, 2019.
Opinions expressed in this article are not necessarily those of bioMerieux, Inc.



My husband had uro sepsis twice within three years.He went into septic shock. The last one was on June 6th.He was aggressively treated with IV antibiotics for almost 2 months. Now, he has prostatitis taking another set of antibiotics. Can he go for a scheduled knee replacement surgery?
Hi Susheela; thank you for your comment! We are sorry to hear about your husband’s situation. However, we cannot give individual medical advice on this blog, so we recommend that you ask your doctor this question.
Best,
The bioMerieux Connection Editors