COVID-19 and Antimicrobial Resistance: Dual Health Threats
By the bioMérieux Editors | Reading time: 4 min
Antimicrobial resistance (AMR) is one of the world’s most serious public health threats. According to a recent study published in The Lancet, bacteria resistant to antibiotics are responsible for 1.3 million direct deaths each year and 5 million indirect ones. The estimations were made in 2019, before the COVID-19 pandemic exacerbates the problem.

Unfortunately, those who are the most vulnerable to the SARS-CoV-2 virus, which causes COVID-19, are also the most vulnerable to drug-resistant infections. People over the age of 65 and those with underlying medical conditions like cardiovascular disease, diabetes, chronic respiratory disease, and cancer are more likely to develop serious illness, no matter the cause.

Many hospitalized COVID-19 patients have been receiving antimicrobials, but relatively few have actually had bacterial co-infections or secondary infections. This means that many antimicrobials may have been administered to patients unnecessarily, therefore contributing to the spread of AMR. Some studies have shown that antibiotics have been administered to the majority of hospitalized COVID-19 patients, and 80-100% of COVID-19 patients in the ICU.

“Since the emergence of COVID-19, collected data have shown an increase in antibiotic use, even though most of the initial illnesses being treated have been from COVID-19 viral infection,” says Dawn Sievert, senior science advisor for antibiotic resistance at the US Centers for Disease Control and Prevention, in an article published in the BMJ. “The resulting increased exposure to healthcare settings and invasive procedures, along with expanded antibiotic use, amplifies the opportunity for resistant pathogens to emerge and spread.”
How Diagnostics Can Help
Diagnostics can help fight COVID-19 and AMR by assisting doctors with treatment decisions. With diagnostics, doctors can determine if a patient has COVID-19, a coinfection, or a secondary infection, and what pathogen is causing the infection. Especially for severe infections, accurate and rapid bloodstream pathogen identification and antimicrobial susceptibility testing can help doctors improve clinical outcomes.

How Vaccines Can Help
Vaccines can help in the fight against COVID-19 and AMR as well. They are critical for preventing infections, including resistant infections. Healthcare providers can help ensure that patients receive the appropriate vaccinations on schedule. Patients should learn about vaccines recommended for all ages and follow their physician’s guidance.

How You Can Help
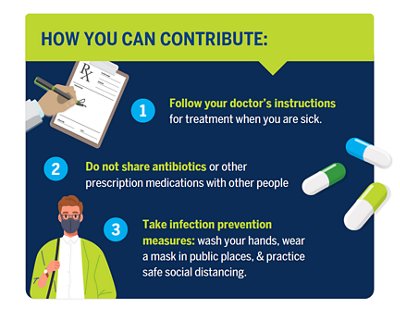
The transmission of COVID-19 and the spread of AMR can also be mitigated with your help. To prevent the transmission of COVID-19, understand how the virus is transmitted. Wash your hands often, wear a mask in public places, and practice social distancing (at least 6 feet away) with people outside your home. The spread of AMR can be curtailed in a number of ways, including through infection prevention measures such as hand washing and the appropriate use of antimicrobials. You should get vaccinated according to your doctor’s recommendations, use antibiotics exactly as they’re prescribed.
It is crucial that we do not overlook the potential for the pandemic to increase AMR around the world. “Before the SARS-CoV-2 pandemic, overcoming AMR already demanded urgent global action,” states a Nature editorial. “Now that we are in the midst of a pandemic, understanding the pathogenesis [how a disease develops] of SARS-CoV-2 infection, and the potential for bacterial coinfections, is imperative.”
DOWNLOAD THE FULL INFOGRAPHIC
- Filename
- 20_AMR-Covid-Infographic_V3c (3).pdf
- Size
- 2 MB
- Format
- application/pdf
SHARE THIS:
- AMR AMS
- Infectious Diseases