How do the COVID-19 tests and molecular tests work?
By Chris Cook, Director of U.S. Medical Affairs at bioMérieux
Reading Time: 5 minutes
Amid the spread of COVID-19, testing for SARS-CoV-2, the virus that causes it, is at the forefront of the battle. Patients rely on test results to confirm if they’ve acquired the coronavirus, and public health entities around globe rely on the data to learn how and where the virus is spreading.
In many parts of the world, tests have been made widely available for patients. In the last two years, the world has learned about PCR not only through the media but also through the shared experience of being swabbed and tested for COVID-19. But do you understand how these tests work?
What Types of Tests Detect COVID-19?
COVID-19 is usually detected with a type of molecular diagnostic test called Real-time Polymerase Chain Reaction (RT-PCR). This type of test is designed to find out if the virus is present by looking for genetic material that is unique to SARS-CoV-2, the virus that causes COVID-19.
How RT-PCR Tests Work
The genetic material of viruses and bacteria is composed of RNA or DNA. SARS-CoV-2 carries its genetic code as RNA. RNA stands for ribonucleic acid and is strung together from molecules called ribonucleotides in a particular order to produce genetic material. DNA stands for deoxyribonucleic acid, and its structure is double-stranded helix, made up of pairs of molecules called nucleotides. DNA and RNA have evolved to work together to make proteins that cells need to survive, so it is possible to copy RNA from DNA and vice versa. RT-PCR tests for COVID-19 take advantage of that ability to detect the SARS-CoV-2 virus’s genetic material.
Step 1: Taking a genetic material sample
At the medical facility or testing center, a medical professional will swab inside your nose to capture a sample containing viruses if they are present. After the swab is removed, it is snapped off at the break line and placed in a sterile vial to be sent to the lab.
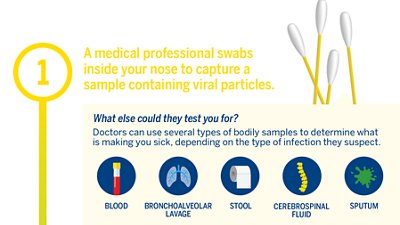
Step 2: Extraction
The next step is the extraction process. Bodily samples are processed in the lab by machines that extract and isolate genetic material to determine which type of virus or bacterium has infected you. The process includes adding different reagents (chemicals) to the sample and repeatedly spinning it in a centrifuge.
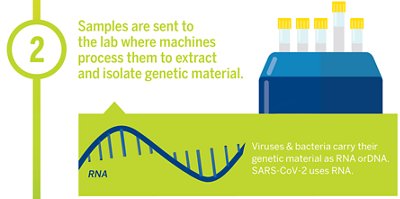
Step 3: Copy DNA from RNA
At the lab, RNA collected from the sample is next combined with the chemical building blocks for DNA, called nucleotides, and a special enzyme that copies the RNA code into DNA. Some viruses and other organisms carry their genetic code as DNA, instead of RNA, so it is not always necessary to copy DNA from RNA. However, for viruses that carry their genetic code as RNA, this sets up the sample for the most important part of the process.

Step 4: DNA Amplification
The new DNA must be amplified (copied) until there is enough to study it. This step is called polymerase chain reaction (PCR). Amplification primers, which are short sequences of DNA unique to a specific virus or other pathogen, are added to the sample along with a special enzyme and other chemicals. During this process, the DNA strands are “unzipped” so that the primers can attempt to match up with the DNA sequences. If the primers don’t match up with DNA in the sample, then the DNA can’t be replicated.
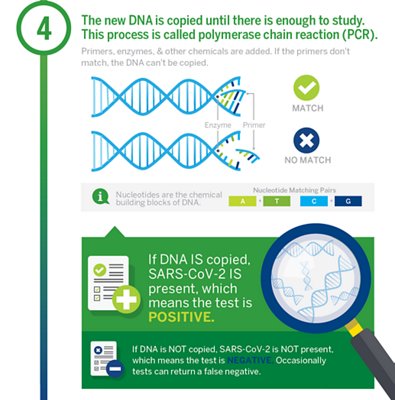
Step 5: Identifying the Result
If there is SARS-CoV-2 in the sample, then the DNA will be replicated, and the test will register a positive result. If there is no SARS-CoV-2 in the sample, then the SARS-CoV-2 primers won’t copy any DNA, and the test will register a negative result. Sometimes, a test will return a false negative result. This can happen for a few reasons, including a low-quality sample, or if the virus wasn’t present in the nasal cavity, as can happen with patients who are asymptomatic. The results of your test(s) will be communicated to your healthcare provider, who will share them with you and provide guidance based on your results and symptoms.

Why Molecular Testing is Important
Over the last decade, molecular testing has become more routine, due to the development of automated instrument systems that provide accurate results utilizing PCR and other molecular detection technologies.. Laboratory results play an important role in medical decision-making and molecular diagnostics have become a crucial component of life-saving patient care.
DOWNLOAD THE FULL MOLECULAR TESTING INFOGRAPHIC
- Filename
- 20-Covid-19-Testing-Infographic-V1d (1).pdf
- Size
- 8 MB
- Format
- application/pdf
SHARE THIS:
- Infectious Diseases